Researchers used data from over 71,000 health records to help identify a definition for treatment-resistant depression (TRD). They found that 2+ switches between antidepressants and/or augmented treatment produced a close approximation of treatment-resistant depression, suitable for use in future research.
Around a third of individuals living with depression experience treatment-resistant depression (TRD), which does not respond to antidepressants, even after several different ones have been tried.
Researchers would like to identify and study people with TRD, so they can develop better treatments, but this is hard to do because health record data contains limited information about how the patients feel.
Instead, researchers usually try to estimate TRD from the number of switches between antidepressant medications. However, current definitions of TRD do not take into account complex real-world prescribing events, such as augmentation (combining antidepressants with antipsychotics or other medications) or the significance of a switch between antidepressant classes (which is more likely to indicate that it isn’t working, rather than a switch within class due to side effects).
In this study, researchers analysed health records within DataLoch, a service that enables safe, secure access to de-identified health data from the South-East Scotland. Researchers then repeated these analyses in Generation Scotland and UK Biobank, two consented cohort studies where participants volunteer health-related information. They looked for health record codes indicating depression and any subsequent antidepressant prescriptions. They then examined nine definitions of TRD to identify the most balanced and useful one for future research.
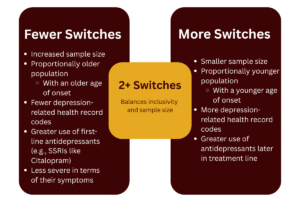
Researchers found that when they applied a definition of TRD that included those with 2+ switches or augmentations to each sample, it balanced sample size with depression severity. However, the researchers recommend viewing treatment resistance as a continuum whenever possible.
This study also highlighted that TRD is underrepresented in current volunteer cohorts due to healthy participation bias and that further studies are needed. Using prescribing/dispensing data to define TRD creates a more representative definition, reflective of real-world treatment, that can be easily reused by other researchers.
Link to Journal Article:
Iveson, M.H., Ball, E.L., Lo, C.W.H. et al. Treatment resistant depression in electronic health records: definitions matter. BMC Psychiatry (2026). https://doi.org/10.1186/s12888-026-08085-y
Elizabeth Thomas worked with Matthew Iveson and Iona Beange on this lay summary as part of her placement for the MSc in Science Communication and Public Engagement, University of Edinburgh