Neural tube defects?? What exactly are they and why is it important?
These were questions I had when I first learned that reducing neural tube reductions held the top spot in the 2018 report by the Public Health Association of Australia, Top 10 Public Health Successes Over the Past 20 Years.
So, what exactly is a neural tube defect (also known as NTD), and why does it matter?
As the report states, “neural tube defects (anencephaly, spina bifida, encephalocoele) are severe birth defects, with high mortality and lifelong morbidity. They are a major cause of perinatal and infant death, and were estimated to cause 71,000 deaths globally in 2010.”1 Additionally, researchers Lo, Polsek and Sidhu found that NTDs may present life–long economic problems, especially to poor families. Which is of particular importance as they also showed that low and middle-income countries are likely to have a NTD burden twice the rate of high-income countries.2
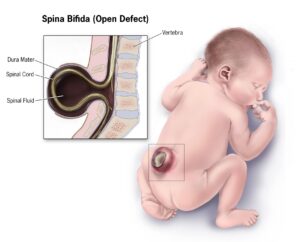
Learning about these conditions made me think about a young patient I once saw in Haiti with spina bifida and how the condition will affect him and his family for the rest of their lives. Was it preventable? Can all countries reduce the prevalence of these types of birth defects? How did Australia go about doing so?
It turns out, that many neural tube defects can be prevented when women of reproductive age consume an appropriate daily amount of folic acid.3 And it appears that is exactly what Australia did. In 2009, a mandate was established that required the addition of folic acid to wheat flour bread making. During the period to follow from 2009 to 2016, Australia was able to reduce neural tube defects by 14% across their total population and by 74% among Indigenous Australians.1
I find this successful public health effort fascinating for many reasons, but what stands out the most is the comprehensive approach taken. Rather than focusing solely on how to treat and care for children born with neural tube defects (the “symptom” of maternal nutritional deficiency), the program focused on ensuring that all potential mothers had sufficient nutritional health to prevent the condition in the first place (addressing the “root cause” of NTDs).
When looking at this issue through the approach of planetary health solutions (defined as examining the health effects associated with changes to a natural system and then taking a collaborative, interdisciplinary approach to optimize health outcomes),4 I have even more questions than when I first read the report on neural tube defects. Was the birth of the little boy I saw years ago with spina bifida affected by poor nutrition in his mother? Was this poor nutrition related to a lack low crop diversity in her area? Was the low crop diversity connected to deforestation and/or climate change?
I certainly don’t have the answers, but I look forward to exploring these questions and topics as we progress and learn through this Global Health Challenges course.
Citations:
1. Public Health Association of Australia (2018) Top 10 public health successes over the last 20 years. Available at: https://www.phaa.net.au/documents/item/3241 (Accessed: Sept. 27th, 2020).
2. Lo, A., Polšek, D., & Sidhu, S. (2014) ‘Estimating the burden of neural tube defects in low- and middle-income countries’, Journal of global health, 4(1)-010402, p.1-9. Available at: https://doi.org/10.7189/jogh.04.010402 (Accessed: Sept. 27, 2020).
3. WHO Guideline At-A-Glance: Optimal Blood Folate Concentrations for the Prevention of Neural Tube Defects (2017) Available at: https://www.cdc.gov/ncbddd/birthdefectscount/obf-guideline.html (accessed Sept. 27th, 2020).
4. Myers, S. (2017) ‘Planetary health: protecting human health on a rapidly changing planet’, The Lancet, 290(Dec.23/30), p.2860-2868.
Photo source: https://www.houstonchronicle.com/local/prognosis/article/Umbilical-cord-patch-good-for-fetal-spina-bifida-8354902.php


Kevin,
I am particularly interested in Maternal and child nutrition so I really enjoyed reading this. I agree with you, it seems like Australia got to the root of the problem when looking for solutions instead of simply treating the symptom. Thanks for bringing the awareness and highlighting the public health solution that Australia has implemented! It would be amazing to see this and other nutrition challenges tackled by other countries!
Katie
Thanks for reading Katie!
This is a great post, Kevin. I had no knowledge of the prevalence of neural tube defects in Australia. I am also buoyed by the response taken. Were Indigenous communities reporting more cases of the condition, I imagine?
Thanks,
Ladeisha
While I haven’t seen the exact numbers, that seems to be the case. According to the report, “Voluntary fortification of some foods was approved in 1995. However by 2001 few foods were fortified so the gains were limited. A 30% reduction in neural tube defects was seen following health promotion of supplement use and voluntary fortification, but not across all ethnic and socioeconomic groups. In particular, there was no effect on the prevalence of neural tube defects in Aboriginal infants, who already had a higher rate, and hence the gap between Aboriginal and non-Aboriginal rates widened.”
Which to me shows the success of the program being even more impressive. After having some success with voluntary fortification, it is only when the mandatory fortification went into effect that the underserved populations were better served. Seems like a great adaption/improvement to their program.
I really enjoyed reading the blog Kevin – from the title through the end, you make a strong argument. I agree with Katie in that it is great to read about the solution and also the drivers on how they got to the problem. Especially as the reduction of the problem is so much larger in the Aboriginal population than in the non-Aboriginal. My immediate thought is because the problem was so much more prevalent in the former than in the latter. This leaves me wondering if the gap in the burden of disease between these two populations has narrowed? Thanks for sharing! Evelyn
Hi Evelyn. This was a great question (by you and Ladeisha) that made me dig a little deeper. And to somewhat surprise, the disease burden gap was actually flipped!
According to the full report, Monitoring the health impacts of mandatory folic acid and
iodine fortification, by the Australian Institute of Health and Welfare: “During the pre-fortification period, the rate of NTDs among Indigenous women was at least 80% higher than among non-Indigenous women (111% higher in the total study population and 88% higher in the population omitting NSW residents). The trend was reversed in the post-fortification period, where the rate of NTDs among Indigenous women was at least 40% lower than among non-Indigenous women.”
*There is a great graph showing these results on p. 40 of the report, figure 2.24. The report can be found here: https://www.aihw.gov.au/getmedia/6bfafa4a-2255-4f04-8955-7496c9e5b2c1/19192.pdf.aspx?inline=true
Hi Kevin,
An insightful post with a lovely presentation of how policy development, policy implementation and research can drastically change healthcare outcomes. Mostly I am glad that it shows that interventions do not have to be overly complicated as a simple addition to bread could cause a large cascade of decreased cases over years.
Great point Beatty. Thanks for your comments!